2022/01/28 | Research | Biomechanics
Implantation position influences turbulence in TAV
For the complication-free long-term functioning of artificial heart valves, they should reproduce physiological blood flow with as little turbulence as possible, because turbulent blood flow may contribute to blood clot formation and early valve deterioration. The ARTORG Cardiovascular Engineering (CVE) lab has now compared two implantation positions for transcatheter aortic valves (TAV) with respect to their effect on turbulent blood flow. The results show that careful patient-specific implantation planning could lead to reduced turbulence.
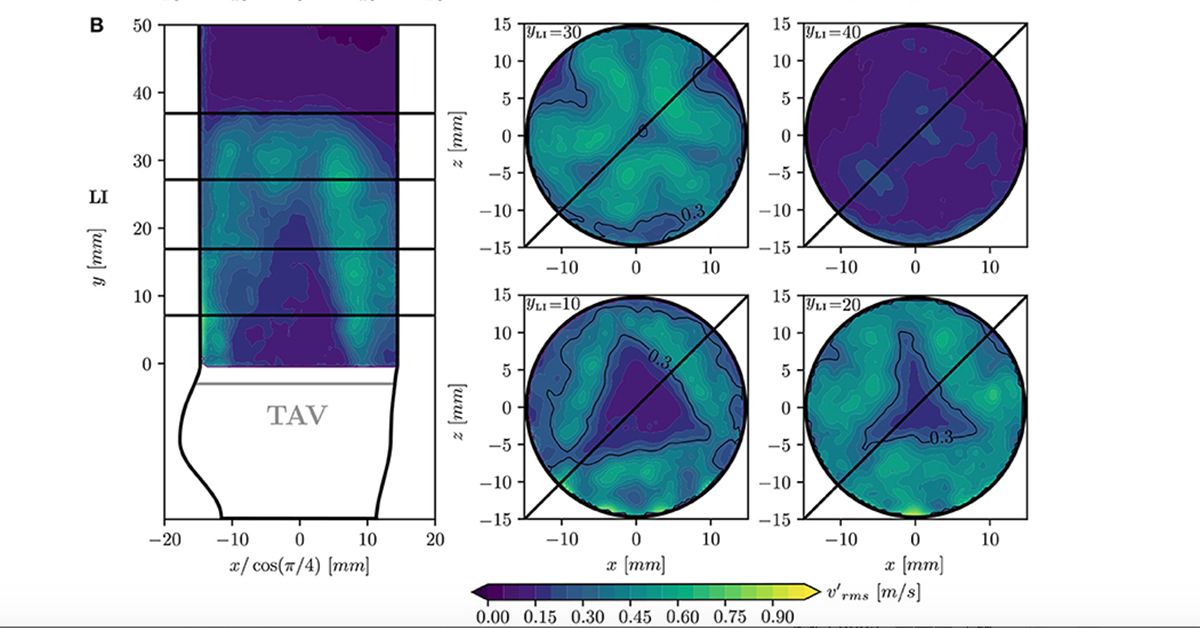 Root mean square of velocity fluctuations v′rms in different cross-sections of the flow-domain for lower implantation with approximately 8% higher turbulence intensity than an upper implantation of a transcatheter aortic valve.
(https://doi.org/10.3389/fcvm.2021.804565)
Root mean square of velocity fluctuations v′rms in different cross-sections of the flow-domain for lower implantation with approximately 8% higher turbulence intensity than an upper implantation of a transcatheter aortic valve.
(https://doi.org/10.3389/fcvm.2021.804565)
As the minimally invasive implantation of catheter-delivered self-expanding artificial heart valves becomes available to a wider population of lower risk patients, insights into optimal transcatheter aortic valve implantation (TAVI) receive a heightened interest. The ARTORG CVE lab has specialized in studying blood flow characteristics with experimental setups and has now compared the turbulent flow dynamics with an upper as compared to a lower implantation position for TAV.
Tests were conducted in a pulse replicator and the three-dimensional flow field was extracted by means of tomographic particle image velocimetry. The team compared fluctuating velocities and turbulent kinetic energy between the two implantations and derived velocity spectra at different spatial positions in the turbulent wakes to characterize the turbulent flow. Results showed that the currently recommended lower implantation caused approximately 8% higher turbulence intensity as the valve revealed smaller opening area and more corrugated leaflets during systole, as well as more accentuated pinwheeling during diastole which are likely due to the incomplete TAV expansion in this implantation position.
As intensified turbulent flows could contribute to the TAV's structural deterioration, a specific intervention planning targeted to the patient’s aortic root geometry and calcification degree could help prevent incomplete TAV expansion and foster the longevity of the artificial heart valve.